‘Sometimes, postnatal mothers use the floor to rest immediately after delivery because beds in postnatal wards are in extreme shortage’
By Kebba Jeffang
Shortage of beds has hit most healthcare facilities in the Upper River Region. Consequently, patients in critical condition including postnatal mothers are compelled to use mattresses on the floor to rest after delivery while only a few trained nurses are available-struggling to give a day-to-day care to patients. The realities of the health provision are unmatched with the National Health Policy 2013-2020 objectives.
Basse is the administrative town of Upper River Region. It is about 375 kilometers from the capital, Banjul. The entire region with a population of 239, 916 has no hospital except what is now called the ‘Basse district hospital’ which is below standard in every aspect of health care delivery.
Like urban areas, drugs are also largely unavailable at these facilities. Speaking to some natives in Sandu, Wuli, Kantora and Basse all in URR, they claimed that they are ‘neglected and forgotten.’
Access to health facilities is also a major problem- a nightmare for pregnant women who sometimes deliver on donkey carts before getting to a midwife at the closest health post, villagers said.
The current realities in various health facilities regarding beds in rural Gambia have failed to meet more than 75 percent of the policy target.

“The number of beds available compared to our admission capacity is far less. You cannot allow certain patients with critical cases to go home like that and you can only place mattresses on the ground for them to sleep which is not ideal,” the facility’s Officer-In-Charge Kemo Badjie said.
Ideally, he said, each patient in the health centre should have a bed.
In The Gambia, the major health centres serve as the referral point for minor health centres for services such as comprehensive emergency obstetric care (surgical, blood transfusion services and further medical care as per the national health policy NHP). The standard bed capacity for a major health centre ranges from 110 -150 beds per 150,000 – 200,000 population.
The policy also outlined that a minor health centre is the unit for the delivery of basic health services including basic emergency obstetric care. The national standard for a minor health centre is 20-40 beds per 15,000 populations. They are tasked to provide up to 70 percent of the basic health care package needs of the population.
Yero Bawol health centre is situated in Wuli West, 14 kilometers from Basse. It receives on average 60 to 70 patients daily from all catchment areas, according to the Centre’s record.
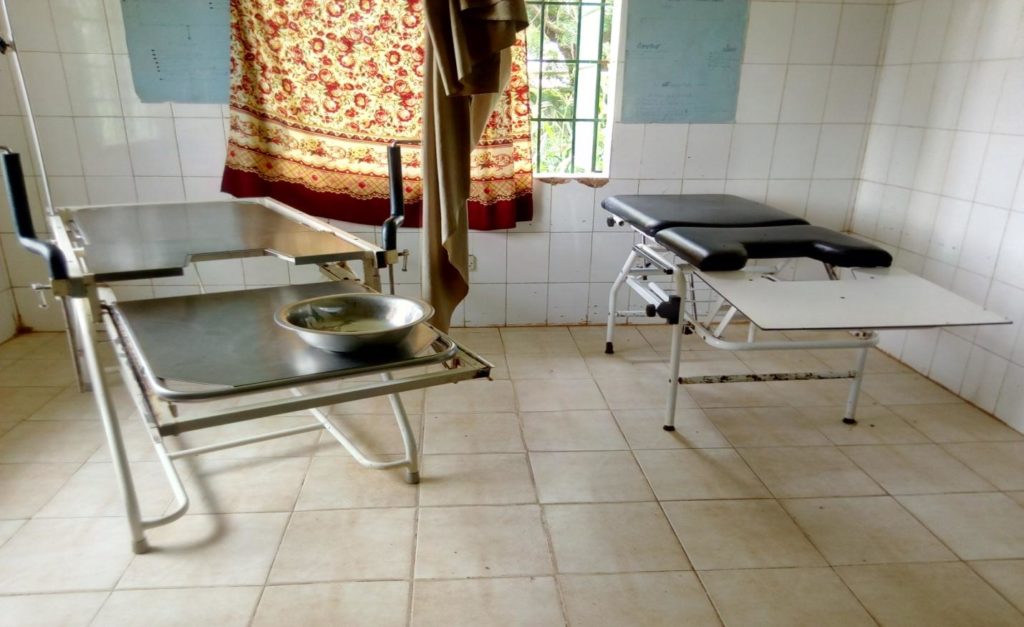
The facility has only six beds in the postnatal ward. An empty ward was also seen and therefore not in use due to lack of beds.

According to Badjie, the beds that are available in the ward are in their worst condition and almost unfit for purpose. He said if things are normal, each patient should have his or her own bed.
“As I’m speaking now, two women are already in the labour ward and they do not have beds. On average, the facility records 60 to 70 patients each day from catchment areas,” he said.
At Diabugu health centre in Sandu, some of the pregnant women who are about to deliver are usually referred to the region’s major health centre due to shortage of beds for them to deliver on.
“Due to bed inadequacy, when the birth rate is higher, we refer pregnant women who are already in labour to Basse district hospital and there are possibilities that some could deliver on the way,” Karamo Manjang, the Officer-In-Charge disclosed.
He said the facility has only two beds for delivery purpose- against a daily average of four deliveries. He said there are dangers attached to such referrals considering that they could deliver on the way which is not convenient and could even lead to death. Manjang also lamented that the Diabugu health centre has only two beds reserved for the postnatal ward.
The district of Sandu has a total population of around 25, 525 people.
“The female ward has four beds, male ward has five. Sometimes we use these two wards for postnatal mothers,” Manjang said.
The National Development Plan (NDP) of the Barrow-led coalition government which was recently launched stressed the need for a strong primary healthcare as the inherited one “is no longer able to serve the population adequately.”
However, the government is showing no sign of urgency to improve the condition for the rural patients after almost two years in office.
The vision of NHP is to provide quality and affordable health services for all by 2020 while it has a mission of promoting and protecting the health of the population through the equitable provision of quality healthcare.
Tiring nurses in charge of lives
“Here in Yero Bawol, we work almost 24 hours in order to meet the demand of the people due to shortage of nurses. We have only three trained qualified nurses and two untrained. This means we have only five nurses in this whole facility including me as the OIC,” Badjie said.
He said statistics have shown that more nurses are posted in the urban area than the rural areas which he thinks should be reviewed.
He said: “Unless we redistribute the nurses fairly, we will never be able to meet the demand of this area.”
The health policy states that provision of health care shall be based on comparative need.
Badjie believes that most trained nurses turned down rural transfers due to several factors including abysmal pay with poor allowances.
At the Fatoto health centre in Kantora, about 42 km from Basse, there are only four trained staff and one midwife. A source at the facility said nurses are overstretched to work 24 hours due to limited staff capacity.
Diabugu health centre also has only two midwives, two general nurses and one eye specialist, the authorities said.
The policy emphasizes the affordability and adequate staffing in health facilities while the country’s three year blue print tasked the government to ensure that “appropriately skilled workforce is in place” to reduce maternal and newborn mortality and reduce the burden of communicable and non-communicable diseases.
Pregnant women referred in ‘pickup vehicles’
All the health centres in the Upper River Region refer patients to Basse district hospital which is tens of kilometers away. With one ambulance allocated to almost all facilities, some patients, including women in labour, are compelled to board pickup vehicles for referral purposes.
The Diabugu authorities said some patients who are referred to Basse have died possibly due to road condition and lack of drugs.
Diabugu health centre was established 10 years ago and it visibly needs renovation. Some of the staff at the health centre said they live with the natives due to housing constraints.
Women delivering on carts
The regions’ roads connecting villages to the metropolitan town are in dilapidated condition. This affects Wuli, Sandu, Tumana, Jimara and Kantora districts.
Jannah Suwai, a woman believed to be in her 50s, was met at Yero Bawol health centre. She accompanied a pregnant woman for delivery from Fadiya Kunda using a 3 wheels vehicle locally called ‘batch car.’ The lady delivered safely the following morning.
“We are really suffering. We paid the batch car D350 for a very short distance. Our situation is a complicated one because if you are sick, accessing health facilities is a problem. If you are in labour, to reach the health centre is another big challenge,” she decried.
The situation is worse in some parts of Jimara, the president’s home district where sick persons and pregnant women are said to be transported by motorbikes.
A youth leader and a resident of Sifula Sunaalso village, Amadou G. Sowe said the road condition is unbearable especially during rainy season.
“My village is about six kilometers from the main road, Mankamang-Kunda, home of President Adama Barrow and it is difficult to ply especially when it rains. People are seriously affected,” he said.
Sowe said some pregnant women deliver on the road before reaching the highway.
“We use motorbikes, donkey and horse carts to carry women who are in labour to the main road. Sometimes we seek assistance for vehicles from neighboring villages,” he said.
Manjang in Diabugu also confirmed that women deliver at homes due to difficulties in accessing the health facility. He attributed this to bad road condition.
However, the engineers were seen along Wuli-Sandu highway constructing the road that connects the districts to Basse although Jimara is yet to be dealt with.
No money, no drugs
“The issue of pharmacy is that if you don’t have money you don’t get drugs even if you are about to die,” Amadou said.
He said the entire ward depends on pharmacies because there is no health centre in the whole Jimara district.
“Bansang is the general hospital and Basse is a district hospital. People are complaining everyday especially with many people not mobile,” he said
Badjie in Wuli could not deny the drug shortage at the facility. He said Yero Bawol is hard-hit by the lack of drugs especially in the last six months.
According to him, they are assisted mainly by the Resource Based Financing (RBF) project as far as drugs are concerned.

“There is a particular percentage that is captured for drugs and medical items within the project. It has been helping a lot,” he said.
RBF project is run under National Nutrition Agency (NaNA).
“To be candid, drugs are in short supply. The frequency of drug supply is not bad but the quality is most of the times a problem,” he said.
The 2018 budget has allocated D852, 671, 920 to the health ministry, which realized an increment from D794, 867 (amounts in millions) in the previous year. Among the objectives is to improve health services in the country.
But Badjie disclosed that the drug shortage includes Paracetamol tablet in the last six months at his facility.
The NDP commits the government to invest on people through improved health services.
The government will prioritize further investments to develop the country’s human capital. It will do so by ensuring quality health and education, making basic social services accessible and affordable to all, the document stated.
Sanitary concerns at Basse district hospital
The referral centre for the regional health centres has been blamed for lacking basic sanitary standard. The patients said it has been compromised to their detriment.

“I think we are forgotten here. This hospital doesn’t only lack drugs but sanitary standard has also been highly compromised to the detriment of patients. This is how we are being treated here,” said Yaya who prefers not to tell his last name.
He recalled the moment he was admitted at the facility and had to forcefully quit due to conditions of toilets.
“I was admitted here last year before Tobaski. I forced nurses to release me because I was going to die if I should continue inhaling the bad odour that was emanating from the toilets. He had to release me because he understood my concern,” Yaya said.
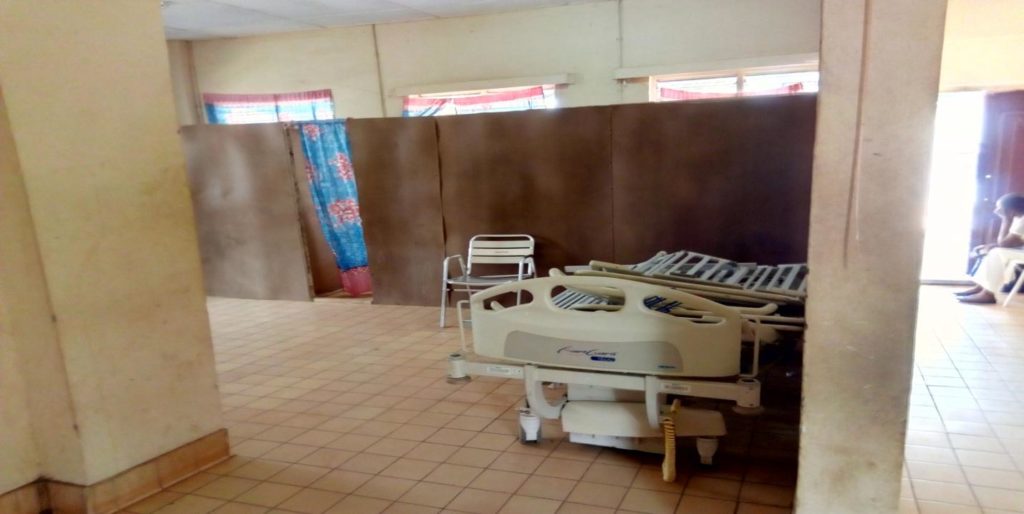
At Basse hospital, some of the wards at the hospital are visibly not in order. One of the wards was partitioned with cardboards with some dismantled beds that weren’t in use. Patients were seen outside the complex with their bodies exposed to heat waves.
The hospital is also said to be confronted with lack of standard equipment.
Nurses who were approached at the said facility to share the conditions of services declined to comment citing some laid down protocols.
The Officer in Charge of Basse district hospital, the director of regional health and director of health services have all declined to comment.
The permanent secretary’s office was visited twice for comment but never materialized.